Insurers across lines of business plan to increase their use of agile development in 2018, according to a new Novarica Research Council survey, "Insurance IT Practices and Disciplines."
However, carriers continue to report struggles with recruiting IT staff to support these new initiatives, according to the survey of 93 insurance company CIOs. Insurers' legacy environments and cultural challenges make attracting new staff difficult, carriers say. The age of existing insurance company systems also has negative impacts on IT cost structure and budgets.
"The range of challenges facing carriers has remained consistent from 2017," writes study author Chuck Ruzicka, VP of research and consulting for Novarica. "Legacy environments pose staffing challenges like retaining resources skilled in managing antiquated systems and finding new employees to replace retiring resources. Acquiring sufficient talent to support new technological initiatives like big data is also a challenge."
The survey asked insurers to rank their adoption rates and expansion plans for key IT practices like:
- Agile development
- QA/testing
- MDM and data stewardship
- Enterprise architecture
- IT governance
- User experience (UX) and human factors engineering
- Bimodal IT or FAST/CORE IT
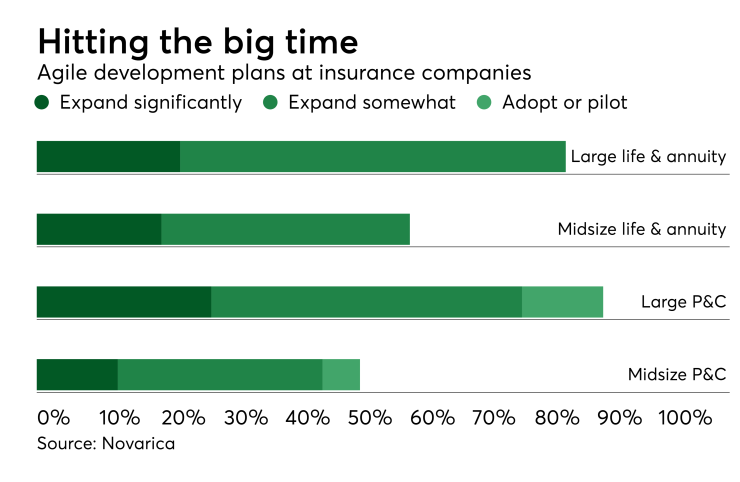
More than half of all respondents plan to adopt, pilot, or expand their use of agile this year; an across-the-board increase most notable among life and annuity carriers. On the other end of the spectrum, transitioning to FAST IT models that encourage experimentation rather than regimentation in the IT department is least popular among the survey group, with only about a quarter of CIOs planning to deploy it at all.
"Like agile, FAST IT requires a new approach to IT processes," Ruzicka explains. "Often, global change is difficult, as the complexity of organizations and the inertia of ingrained processes provide initial resistance that can be difficult to overcome."









